Bipolar Disorder Test: Distinguishing Bipolar Disorder from PTSD Symptoms
November 27, 2025 | By Leo Vance
Have you ever wondered whether your emotional challenges stem from bipolar disorder or trauma responses? Many people struggling with intense mood swings and emotional reactivity find themselves confused between these two conditions. While they share surprising symptom similarities, understanding their distinct origins and patterns is crucial for getting the right support. If you're seeking clarity, a confidential bipolar disorder test can be a valuable first step. Try our free bipolar screening tool today to gain initial insights into your mood patterns.
Understanding Bipolar Disorder: Beyond Mood Swings
Bipolar disorder is defined by pronounced, often spontaneous shifts between emotional extremes that are not necessarily tied to external events. These distinct periods, or "episodes," create a cyclical pattern of highs and lows.
Key Mood Patterns in Bipolar Disorder
- Manic/Hypomanic Episodes: Periods lasting several days or weeks that feature elevated energy, a reduced need for sleep, racing thoughts, and sometimes impulsive or risky behaviors. Bipolar I involves full manic episodes, while Bipolar II is characterized by milder hypomanic episodes.
- Depressive Episodes: Extended periods of persistent sadness, fatigue, loss of interest in activities, and feelings of hopelessness.
A scientifically-designed screening tool, like the one we offer, evaluates these key indicators by assessing the frequency and duration of elevated mood states, changes in energy levels, and the overall impact of these shifts on your life. Take our confidential bipolar screening questionnaire to identify patterns that may warrant a professional evaluation.
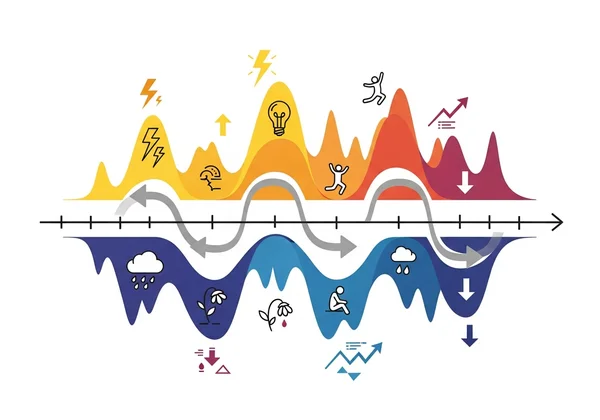
Understanding PTSD: When Trauma Rewires the Brain
Post-Traumatic Stress Disorder (PTSD) develops after exposure to a traumatic event and is fundamentally a trauma- and stressor-related disorder. Its symptoms reflect the nervous system's adaptation to a perceived threat.
Core Symptoms of PTSD
- Hyperarousal: A constant state of being "on alert" or in "fight-or-flight" mode, leading to irritability and jumpiness.
- Avoidance: Actively steering clear of people, places, or thoughts that are reminders of the trauma.
- Re-experiencing: Intrusive memories, flashbacks, or nightmares related to the event.
- Negative Cognition and Mood: Persistent negative beliefs about oneself or the world, and emotional numbness.
Unlike the internal biological rhythms of bipolar disorder, PTSD symptoms are often activated by environmental triggers and stress, causing emotional reactivity that can be mistaken for mood swings.

Bipolar vs. PTSD: Key Differences and Symptom Overlap
The confusion between bipolar disorder and PTSD is understandable, as several symptoms appear in both conditions, including sleep disturbances, irritability, impulsivity, and difficulty concentrating. However, the core distinction lies in what drives these symptoms.
Triggers vs. Spontaneous Mood Shifts
The most critical difference is the origin of the mood change.
- PTSD symptoms are typically a reaction to a trauma reminder, an anniversary, or a stressful situation that feels similar to the original trauma.
- Bipolar episodes often develop spontaneously, following the brain's internal rhythms, without a clear external trigger.
Additionally, while bipolar disorder involves distinct elevated mood states (mania or hypomania), PTSD does not cause sustained periods of euphoria or grandiosity.
It's also important to note that co-occurrence is possible. Research suggests nearly 20% of people with bipolar disorder also meet the criteria for PTSD. This dual diagnosis requires specialized care, as trauma can worsen mood instability. Our optional AI-powered personalized reports can help untangle these complex interactions by analyzing your symptom timeline. Discover your personalized insights.
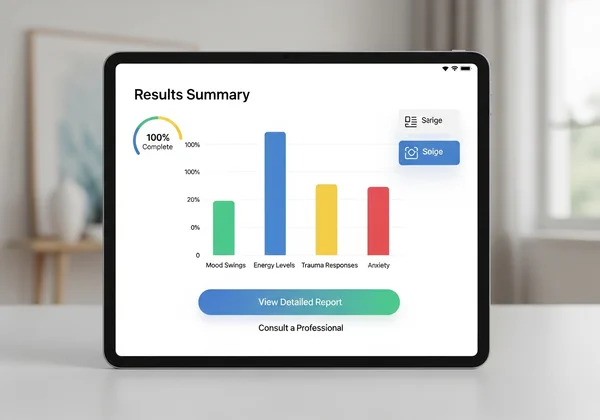
Using a Bipolar Disorder Test for Clarity
While self-assessment is not a substitute for professional diagnosis, a screening tool can provide a structured way to evaluate your symptoms and guide your conversation with a healthcare provider.
What Our Test Assesses (and What It Doesn't)
Our free bipolar disorder test is designed to evaluate criteria aligned with established clinical screeners like the Mood Disorder Questionnaire (MDQ). It specifically looks for patterns suggestive of bipolar cycling and their impact on your daily functioning. It is not designed to diagnose or screen for PTSD, anxiety disorders, or other trauma responses.
If your screening results suggest potential bipolar features but you also have a history of trauma, it's vital to consider both. Observe whether your mood shifts are tied to specific reminders or if they seem to appear without cause. Access your confidential screening results immediately after completing our assessment and share this information with your clinician.
Taking the Next Step on Your Mental Health Journey
Understanding the differences between these conditions empowers you to seek the right kind of help. While our screening tool is a powerful first step toward clarity, only a licensed mental health professional can provide a definitive diagnosis through a comprehensive evaluation.
Use your results as a starting point for a productive conversation with a provider who can review your full symptom history, conduct any necessary assessments, and develop a treatment plan tailored to you. Early and accurate intervention significantly improves outcomes for both conditions. Take that first step now with our secure, science-based screening.
Frequently Asked Questions
Can a bipolar disorder test accurately rule out PTSD?
No, a screening tool cannot provide a definitive diagnosis or rule out other conditions. Our assessment specifically evaluates risk markers for bipolar disorder. PTSD requires separate, trauma-focused evaluations. It is crucial to share your full mental health history, including any trauma, with your provider alongside any screening results.
How do I know if my mood swings are from trauma or bipolar disorder?
Consider these key differentiators:
- Triggers: Do emotional shifts consistently follow trauma reminders?
- Duration: Bipolar episodes typically last for days or weeks at a time.
- Elevated Mood: Does the "high" involve sustained euphoria, grandiosity, and decreased need for sleep? This points more toward bipolar disorder.
- Family History: Bipolar disorder has a stronger genetic component than PTSD.
Our optional AI analysis feature can help identify patterns in your responses that might offer more clarity.
What if I think I might have both conditions?
If you suspect both are present, seek a provider specializing in complex or co-occurring conditions. Treatment will need to be carefully integrated, often focusing on stabilizing mood first while using trauma-informed approaches that won't exacerbate mood symptoms.
Is there one specific test to tell the difference between bipolar and PTSD?
Clinicians use a combination of structured interviews and specific assessment tools rather than a single test. This might include the Mood Disorder Questionnaire (MDQ) for bipolar indicators and the PCL-5 for PTSD symptoms. Our free bipolar disorder test provides initial, bipolar-focused insights that can inform these more comprehensive professional evaluations. Start your confidential screening today.